
Photo by Emma Gossett on Unsplash
Editor's Note: This article discusses reactions to trauma and may be triggering for some readers.
"No other field of medicine in modern times has been buried under such a mudslide of misconception, skepticism, and plain ignorance."
--Steinberg and Schnall, 2001
Many people, including therapists and medical practitioners, find themselves at once fascinated and frightened of Dissociative Identity Disorder or DID (formerly known as Multiple Personality Disorder; Steinberg & Schnall, 2001) In a recent online training, Janina Fisher remarked that the mere mention of the word "dissociation" scares a lot of practitioners (Fisher, 2017).
Many people, including physicians and psychiatrists, associate the term "dissociation" with DID. In turn, many draw their impression of DID from movies, television shows and books that rely on drama and conflict rather than on accuracy. Such portrayals may contribute to myths and fears about DID, rather than fostering empathy for trauma survivors.
In the 1990's, some psychologists proposed that DID isn't a real mental illness. They suggested that therapy clients "enact" the symptoms of DID based on portrayals of the illness in popular media, or that therapists use hypnotic suggestion to elicit DID symptoms (Pierre, 2023). There is little research to support skeptics' theories of DID. In contrast, a body of research does support the trauma model of DID and other dissociative disorders (Loewenstein, 2018). Still, many mental health professionals distance themselves from the entire concept of dissociation due to misconceptions about dissociation and DID in particular.
Currently, DID is considered a mental illness in the DSM-V, with an estimated prevalence of 1.5% in the general population (APA, 2013). A much larger number of individuals are thought to suffer from dissociative disorders (Loewenstein, 2018). Skepicism and biases about DID not only harm those with DID, but also extend to other dissociative disorders and dissociation on the whole.
In an effort to destigmatize DID, other dissociative disorders and "dissociative experiences," some authors have challenged the idea that we should fear DID. Instead, they note that DID represents an extension of common experiences. For example, Steinberg and Shnall (2001) note that about 25% of the general population experiences alterations of consciousness. Richard Schwartz bases his Internal Family Systems approach on the wisdom that we all have parts and that there is much value in looking more closely at our parts (Schwarz, 2021). Others describe DID as part of a continuum of dissociation that includes other trauma designations such as Borderline Personality Disorder and Complex PTSD (e.g., van der Hart, Nijenhuis & Steele, 2006).
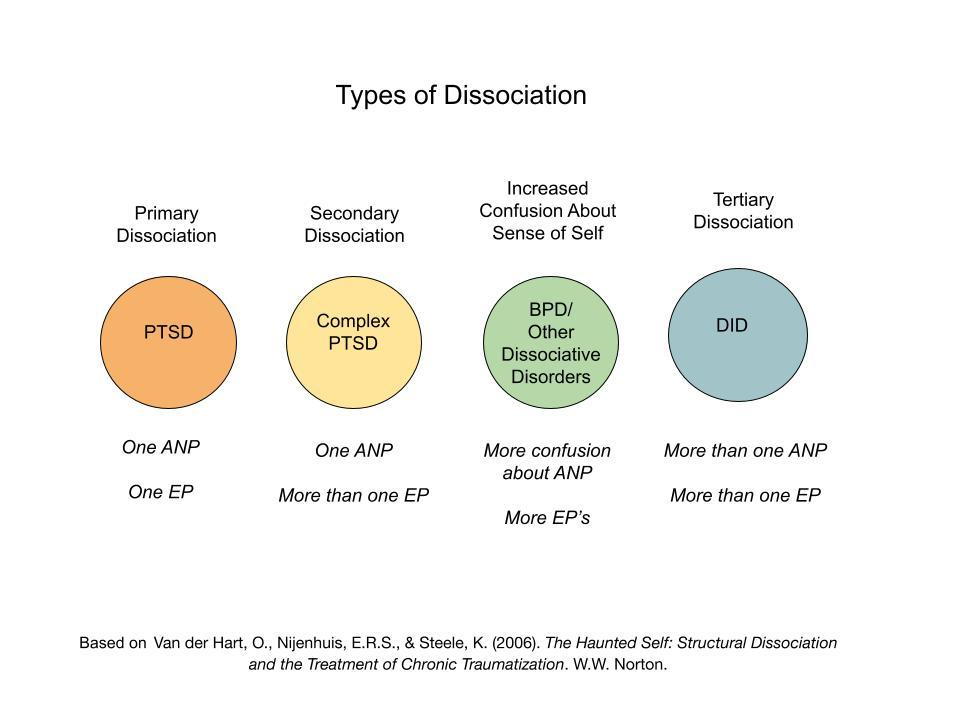
The Structural Dissociation Theory of Personality describes how early and numerous experiences of trauma over time lead to a greater degree of splitting of self. When moving from primary to secondary dissociation, a person develops additional trauma parts (EP's). With additional traumatic stress, the survivor has more confusion about their everyday sense of self (ANP).
With still increasing amounts of trauma, the ANP splits, reflecting tertiary dissociation, or DID (van der Hart, Nijenhuis & Steele, 2006). Although the DSM-V focuses on the idea that DID involves multiple well-formed personalities (APA, 2013). , van der Hart, Nijenhuis and Steele (2006) found that individuals with DID have numerous trauma personalities (EP's) that do not differ greatly from the EP's found in other dissociative and post-traumatic stress disorders.
Therapies based on parts work, such as IFS (Schwartz, 2021), owe a great deal to those with DID. The distinctiveness of personalities commonly found in DID illuminated the idea that all of us have parts and that working with parts helps survivors heal from trauma.
For now, this is the last of my articles expanding on the First Pathway. In my next article, I expand further on the Second Pathway to discuss how abuse sets up the biphasic response.
The content of this blog is for informational purposes only and is not intended to diagnose, treat, cure, or prevent any condition or disease. This blog is not intended as a substitute for consultation with a licensed practitioner. Please consult with your own therapist or healthcare provider regarding any suggestions and/or recommendations made in this blog. Although the author has made every effort to ensure that the information in this blog was correct at publication time and while this publication is designed to provide accurate information in regard to the subject mater covered, the author assumes no responsibility for errors, inaccuracies, omissions, or any other inconsistencies herein and hereby disclaim any liability to any party for any loss, damage, or disruption caused by errors or omissions. Unless otherwise indicated by name or direct reference, any resemblance to persons, living or dead, or actual events is purely coincidental. The use of this blog implies your acceptance of this disclaimer.
American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders (5th ed.).
Fisher, J, (2017). Shame and the Disowned Self: Overcoming Internal Attachment Disorders. Psychotherapy Networker Symposium. [Video] PESI.
Loewenstein, R.J. (2018). Dissociation debates: everything you know is wrong. Dialogues in Clinical Neuroscience. 20(3):229–242. doi: 10.31887/DCNS.2018.20.3/rloewenstein
Pierre, J. (2023). The debate over whether Dissociative Identity Disorder is “real.” Psychology Today. https://www.psychologytoday.com/us/blog/psych-unseen/202302/the-debate-over-whether-dissociative-identity-disorder-is-real
Schwartz, R. (2021). No Bad Parts: Healing Trauma and Restoring Wholeness with the Internal Family System’s Model. Sounds True.
Steinberg, M. & Schnall, M. (2001). The Stranger in the Mirror: Dissociation — The Hidden Epidemic. Harper.
Van der Hart, O., Nijenhuis, E.R.S., & Steele, K. (2006). The Haunted Self: Structural Dissociation and the Treatment of Chronic Traumatization. Norton.
© Nancy B. Sherrod, PhD
